Heel Pain on the First Step in the Morning
The usual cause: Plantar fascia strain from long standing on hard floors and inadequate footwear support.
The goal of this guide: Help you manage it safely and stepwise, without rushing to scans or injections.

Why the First Step Hurts?
Plantar fascia pain has a very typical timing. It often hurts most on the first step after rest, especially after sleep, and then eases once you start walking.
During sleep, the foot often rests in a slightly downward position, so the plantar fascia shortens. Overnight, the body tries to settle small micro tears in that shortened position. In the morning, when you stand, the arch flattens and suddenly stretches the tight, healing tissue. That sudden stretch causes the sharp pain.
What Plantar Fasciitis Is
The plantar fascia is a thick band of tissue under the foot. It runs from the heel bone to the toes and supports the arch, like a strong strap under the foot.
Long standing on hard floors, frequent walking on tiles at home, or footwear without cushioning can overload this tissue. The pain usually comes from irritation where the fascia attaches to the heel, not from the bone itself.
Who Commonly Gets It
- Teachers who stand and walk through the day
- Nurses on long shifts
- Factory and standing job workers
- Retail counter and security duties
- People who walk barefoot on hard floors at home
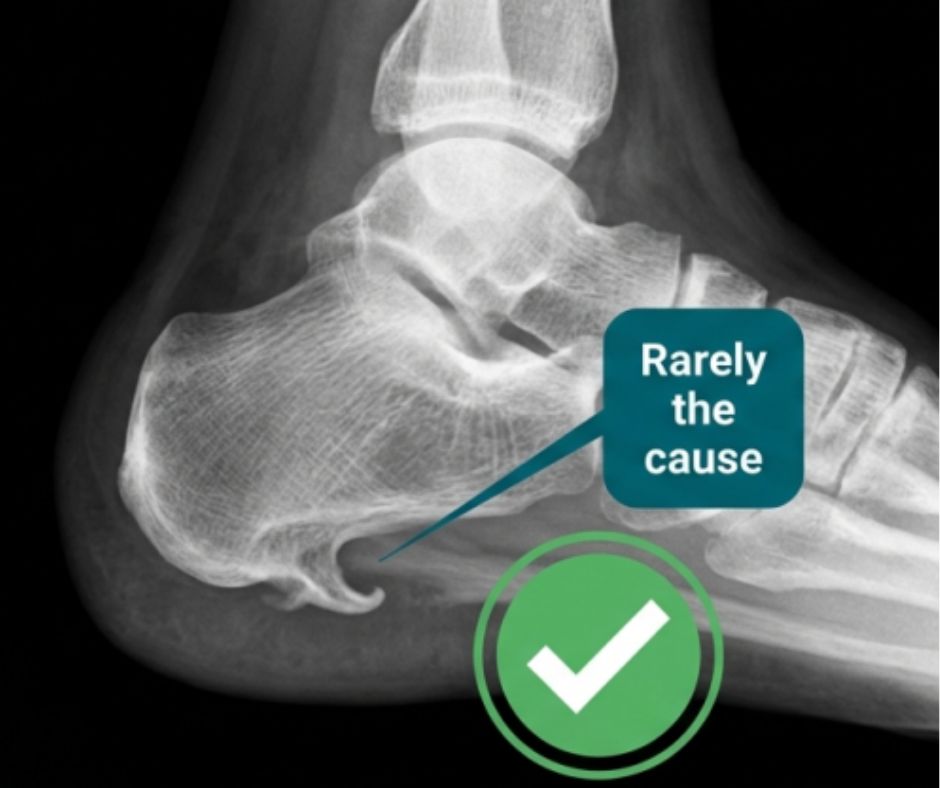
Myth: Heel Spur Is the Cause
Many patients worry after seeing a heel spur on an X ray. The spur is often a sign of long term traction, but it is rarely the main source of pain.
Simple Self Checks
Plantar fasciitis often fits this pattern:
- Pain under the heel, often slightly towards the inner side
- Worst on the first step after sleep, or after sitting for a long break
- Sharp pain first, then a dull ache later in the day
When It May Not Be Plantar Fasciitis
- Burning pain, tingling, or numbness in the foot
- Visible swelling, redness, or warmth around the heel
- Sudden severe pain after a fall or twist
What We Examine in Clinic
The first step is a clinical assessment. Most typical heel pain does not need an MRI.
- Exact tenderness point under the heel
- Calf tightness, which increases heel strain
- Foot arch pattern, flat foot or high arch can overload the fascia
- Walking pattern and footwear wear pattern
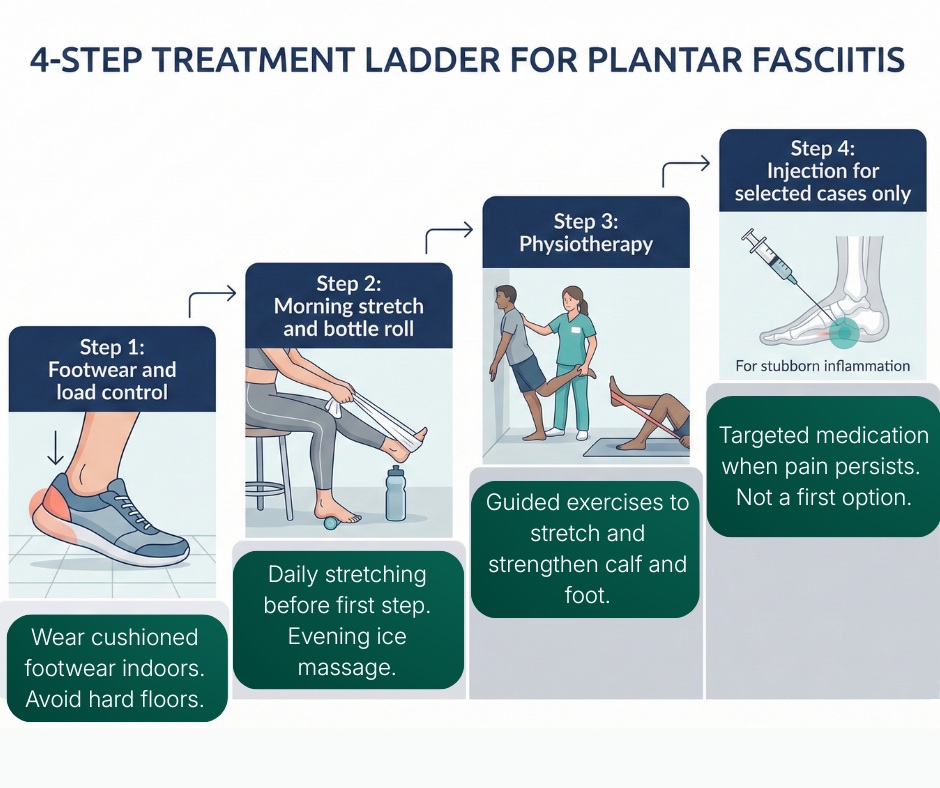
Stepwise Plan That Works
The goal is not to stop life or stop work. The goal is to reduce overload and improve support so the tissue can settle. Most people improve within this four-step plan when followed consistently.
Step 1: Footwear and Load Control
Use cushioning and support to reduce daily heel strain. If you must wear safety shoes, consider a silicone heel cup or a supportive insole. At home, avoid barefoot walking on hard tiles.
Step 2: Morning Stretch and Chilled Bottle Roll
Before getting out of bed, pull the toes up towards you for 20 to 30 seconds and repeat three times. In the evening, roll the foot on a chilled water bottle for 8 to 10 minutes. This combination reduces sudden stretch and helps settle irritation.
Step 3: Physiotherapy if Pain Persists
If pain does not improve after 2 to 3 weeks of consistent home care, supervised physiotherapy helps with: Calf flexibility, Foot mechanics, & Gradual load management. This step is often where recovery accelerates.
Step 4: Injections for Selected Cases Only
If pain continues to block walking or rehabilitation, a targeted injection may be discussed. This is not a first option and works best as part of a structured rehabilitation plan, not as a standalone fix.
When an X ray Is Useful
We usually consider an X ray if:
- Pain started after an injury or fall
- Pain is not improving despite proper conservative care
- We need to rule out a stress fracture or other bone cause
When to See a Specialist?
If heel pain is forcing a limp, affecting work, or not improving with a structured plan, it is worth getting it assessed.
- Persistent pain affecting walking despite 2 to 3 weeks of proper care
- Swelling, redness, or warmth around the heel
- Tingling or numbness in the foot
- Severe limp that starts affecting the knee, hip, or back
Heel Pain Affecting Work or Daily Walking?
A simple assessment can confirm the cause and give a clear, stepwise plan. Most cases are managed without surgery.
Consult with Dr Sumesh Subramanian at OrthoCure Bone & Joint Speciality Clinic, Thirumullaivoyal.
Clinic hours: Monday to Saturday 5:00 PM to 9:00 PM. Sunday 11:00 AM to 1:00 PM.
No. 2, 2nd Street, Santhipuram, Thirumullaivoyal, Chennai 600062.